Home > Get the Facts > Low-Back Pain and CAM
|
Low-Back Pain and CAMFour out of five American adults will experience low-back pain (LBP) at some time in their lives. If you are a health care provider, you have almost certainly cared for such patients. No doubt, some of them have asked you about using complementary and alternative medicine (CAM) to relieve their pain. This article provides an overview of the use of CAM therapies for LBP and lists evidence-based sources for additional information.
A Challenging ConditionLBP is a major public health burden in the United States. It is the leading cause of work-related disability and missed days of work, and the fifth-most-common reason for physician visits. A 2006 report estimated that annual costs of LBP in this country exceed $100 billion. Two-thirds of that is for indirect costs, such as lost wages and reduced productivity. Definitions of nonspecific LBP and its subtypes in the literature vary; a representative definition is in the box below. LBP is often classified either as acute (pain that lasts up to 4 weeks); subacute (pain lasting from 4 to 12 weeks); or chronic (pain lasting for 3 months or longer). Only a small percentage of acute cases of LBP—2 to 7 percent, according to one guideline—become chronic. However, this condition can cause substantial disability and accounts for the majority of LBP-associated costs.
What Is Nonspecific Low-Back Pain?Nonspecific low-back pain is pain occurring primarily in the back with no signs of a serious underlying condition, spinal stenosis or radiculopathy, or another specific spinal cause. Degenerative changes on lumbar imaging correlate poorly with symptoms and are usually considered nonspecific. Condensed from Chou R, Qaseem A, Snow V, et al., 2007.
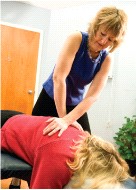
Seeking Options in CAM"Low-back pain is one of our society's most common, burdensome health problems," says Josephine P. Briggs, M.D., Director of NCCAM. "The currently available treatments have limitations. Many patients turn to CAM with the hope of decreasing pain, improving function and quality-of-life, preventing recurrence and chronicity, or avoiding side effects of other treatments." According to the 2007 National Health Interview Survey, back pain is the most common condition for which American adults use CAM. Data suggest that the CAM therapies most frequently used for LBP are chiropractic/manipulation, massage, and acupuncture. Other CAM approaches include yoga, herbal and other dietary supplements, devices, and lifestyle products.
Evaluating Treatment OptionsIdentifying optimal treatment approaches for LBP can be difficult for both patients and clinicians. A thorough patient assessment is the first step for a clinician who may be considering recommending CAM therapies. Clinical practice guidelines stress the importance of ruling out serious underlying conditions and evaluating a patient's psychosocial factors and emotional distress when doing an assessment of LBP. Among recent recommendations on LBP are joint clinical guidelines from the American College of Physicians and the American Pain Society (ACP/APS). Released in 2007, the statement's seven major recommendations to clinicians include:
The ACP/APS guidelines' levels of evidence and net benefit for nonpharmacologic treatments are in: Findings on CAM from Systematic ReviewsSystematic reviews on CAM for LBP may be divided into two categories: Cochrane Systematic Reviews. The Cochrane Collaboration is an international nonprofit organization of health care professionals. Its authors use a systematic process to analyze the results of clinical trials and other sources to explore the evidence for and against the effectiveness and appropriateness of health care treatments. Topics pertaining to CAM for LBP include:
Other Systematic Reviews. The CAM on PubMed database, a service of NCCAM and the National Library of Medicine, provides abstracts of systematic reviews published in peer-reviewed medical and scientific journals. Examples of relevant review topics include:
Two of the themes that are consistent throughout the body of systematic reviews on CAM for LBP are that the evidence evaluated is limited—for example, in its quantity or quality—and that more high-quality research is needed. Specific areas for future research in CAM for LBP include the cost-effectiveness of CAM therapies; head-to-head comparisons of therapies and studies of the effectiveness of CAM therapies versus usual care; and the optimal form, duration, and frequency for treatments. "There is much more to learn about the effectiveness and safety of CAM therapies for chronic LBP and other pain conditions." — Josephine P. Briggs, M.D.
Additional Clinical Considerations: CAM for LBPWhen a health care provider considers treatment options for a patient with LBP, other factors play a part as well, such as clinical experience and the patient's condition, preferences, and expectations. Consider the following additional tips on CAM:
"There is much more to learn about the effectiveness and safety of CAM therapies for chronic LBP and other chronic pain conditions," says Dr. Briggs. "Building a better and clearer evidence base in these areas, and sharing reliable information, are priorities for NCCAM."
Literature Searches In PubMedSelected Citations on Low-Back Pain
NCCAM-Funded Research Results on Low-Back Pain
Sources
|
Copyright 2010 healthalternative.biz
Home Aromatherapy Backgrounders Blog CAM Articles Carpal Tunnel Hoodia Gordonii Green Tea Magnet Therapy About Us Links